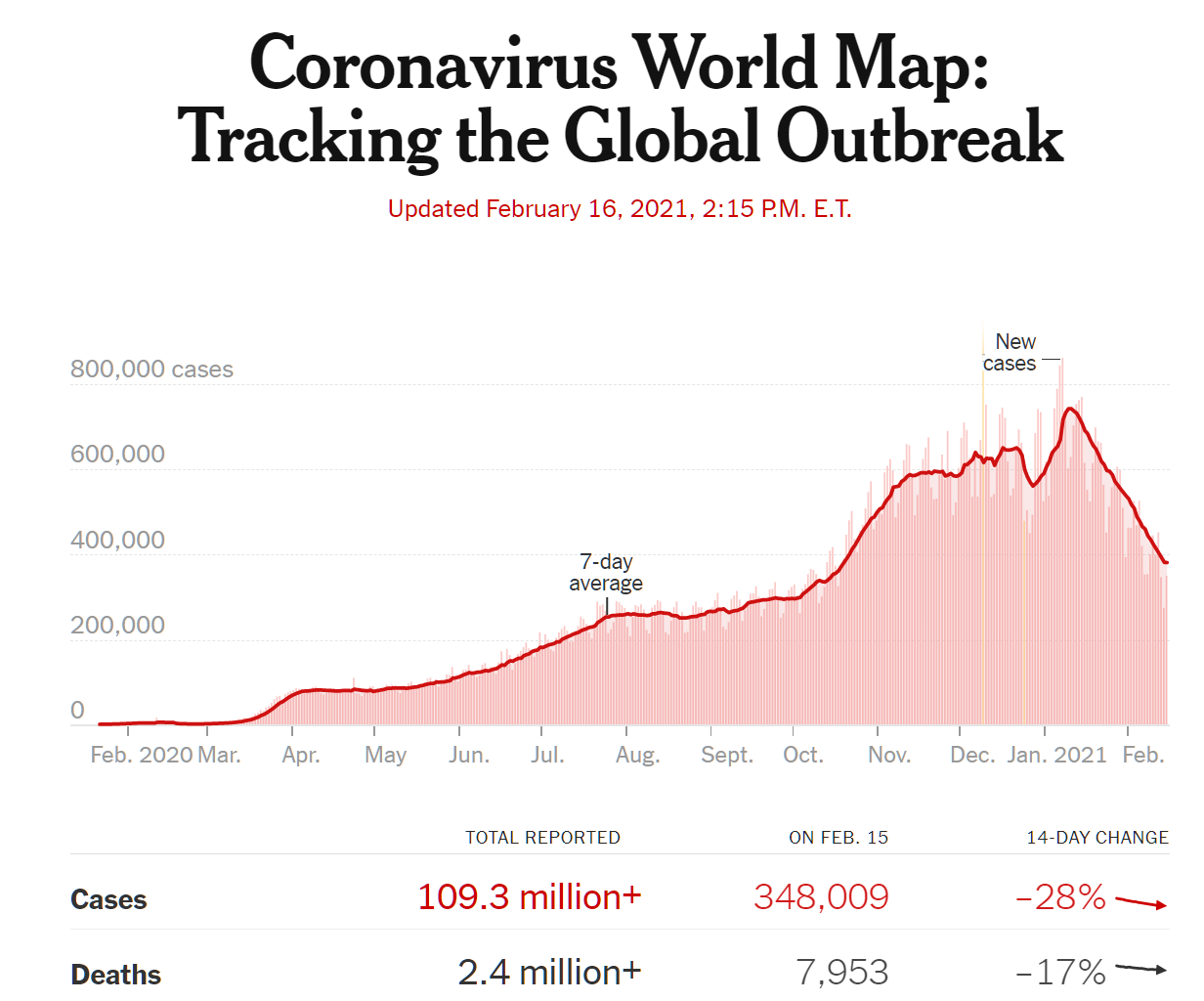
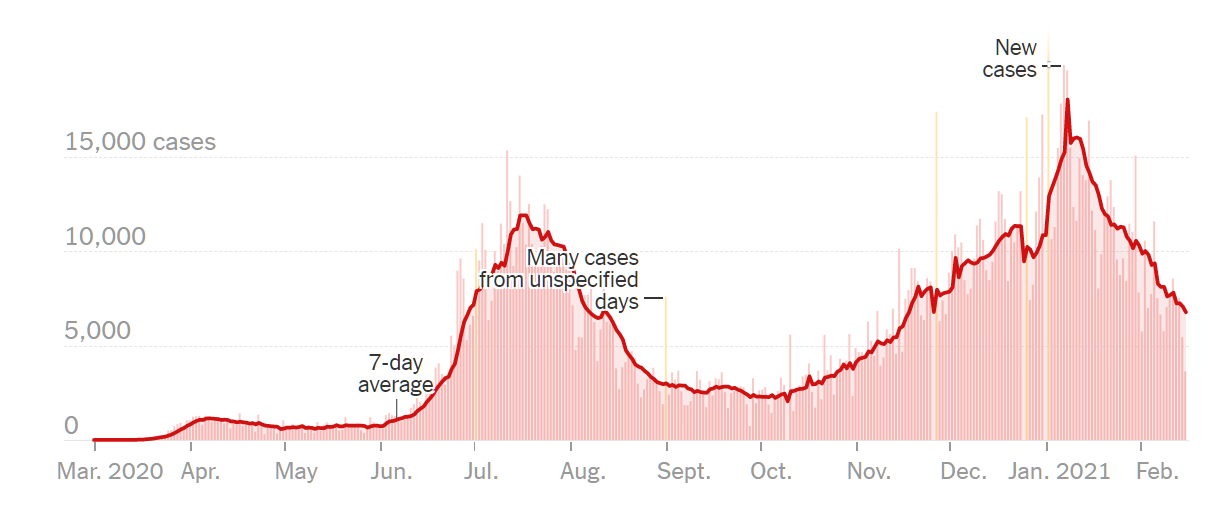
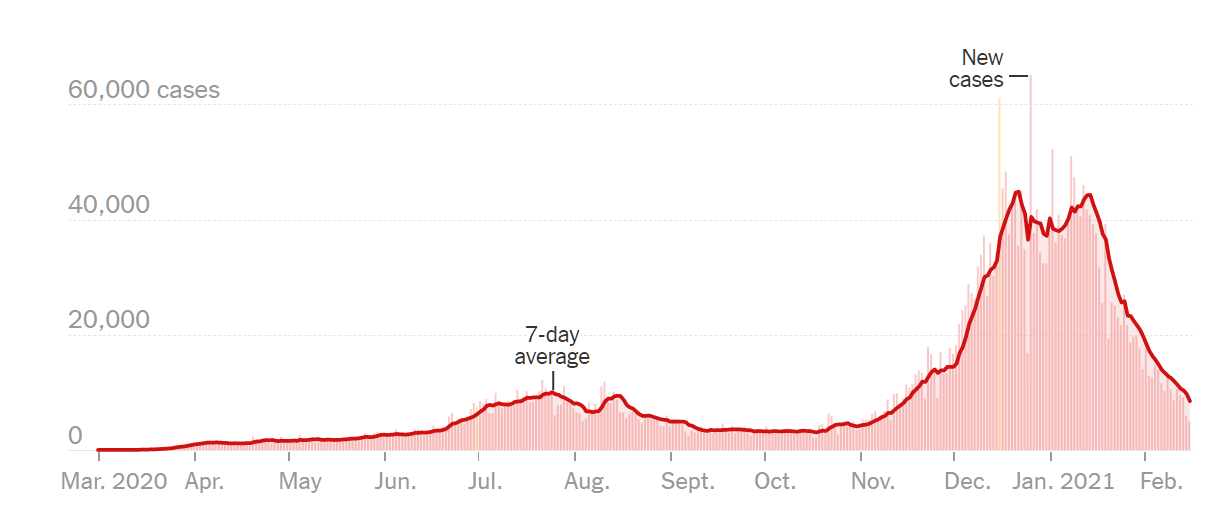
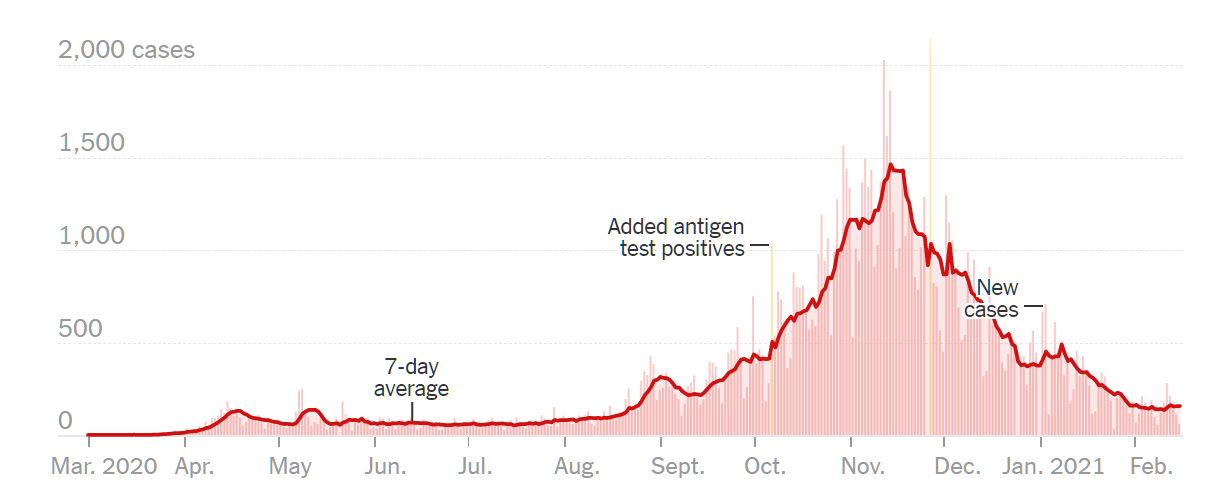
Medical School 2020, Year 3, Week 7 (Pediatrics)
Work starts at 8:00 am at an outpatient pediatric clinic that is a one-hour drive from the hospital. I’m the only student in the clinic. I meet the three attendings, one advanced care provider (“ACP,” typically a PA or NP), and lactation consultant) before the first scheduled office visits at 8:30 am. Two of the attendings are hot off the press, having finished their residencies a year ago. Momma Mabel had a baby in December and is back after three months off [Editor: fully paid thanks to the extra work put in by the childless.]. Her husband is a stay-at-home dad who brings the baby in during lunch. Mercedes Mike, the other new attending who drives a new SLC Roadster, and Busy Belle, a divorced pediatrician in her 50s who is booked weeks out except for two unscheduled daily sick slots.
They have fifteen 15-minute well-child-checks (“WCC”) scheduled each day, thirteen 10-minute scheduled sick visits, and two open 10-minute sick-visit slots at the end of the day. A complicated patient, e.g., chronic headache, may be allocated two 10-minute slots. Five minutes out of the 15 are allotted for rooming. The nurse will get vitals while the physician writes up notes from the previous encounter. The physician then has either 5 or 10 minutes to see the patient without falling behind. I go in with Mabel for a 4-month-old WCC. Mabel invites me to listen to the patient’s heart and I hear an early systolic murmur. When I tell Mabel about that, after the encounter, she says “Yep, good job. That’s called a Still’s murmur. It classically is described as having a musical quality. I didn’t tell the parents because it is a benign murmur of childhood.” Mabel pumps during the one-hour lunch break as I head over to the other side of the office for lunch with Busy Belle.
Belle explains the different pay structures for primary care. Some health systems use a flat salary. “You are required to see a minimum number of patients.” Many health systems are transitioning to a relative value unit (RVU) reimbursement structure. Mercedes Mike stops by and adds: “I considered working for another system that is completely based on RVUs. I’d get paid more per patient, but if I decided to go on vacation for two, I would get nothing. I felt this was a little nerve-wracking for me just starting out with a young family.” Another factor emerging is scorecard evaluation. “We get evaluated based upon peer performance across selected metrics, e.g., smoking cessation, weight loss.”
I shadow Belle for the remainder of the day and we’re done with patients at 4:30 and out the door at 5.
Tuesday I graduate from mere shadowing and begin to interview patients alone prior to the attending coming in. My first interview is with the mother of a 2-year-old presenting for a two-day history of sore throat, fever, and runny nose.The kid just started daycare, and the parents took an ear temperature at 100 degrees, which means she’s technically afebrile because fever starts at 100.4. I complete a physical exam before presenting the findings to Mabel while she fills out an Epic SmartText template. Students are allowed to write notes for surgery, but not for pediatrics due to concerns about insurance reimbursement. We then both go into the room. Either I got the history wrong or the mother has changed her story. The sore throat began three days ago, not two and nasal saline rinse has been used, contradicting my report of no medications. Afterwards, Mabel completes her own physical. We send them home and recommend symptomatic management with Tylenol and ibuprofen if needed.
Our next four patients come in with sniffles or sore throat. I can’t find signs of bacterial infection. “What is your assessment?” asks Mabel. “She has a viral pharyngitis that can be managed symptomatically. Let’s tell them to keep hydrated and make sure there are 3 or 4 wet diapers per day. Return in case of fever.” In the afternoon, I see a 6-month-old with conjunctivitis, bilateral otitis media, and pharyngitis caused by a suspected adenovirus infection. Mabel: “Notice the difference? Treatment is symptomatic, but these kids can get really sick. Tell me the serious complications of adenovirus?” She goes into the next patient while I look at UpToDate. I report that the main complication of adenovirus is pneumonia. Fifteen percent of childhood pneumonias are caused by adenovirus and myocarditis (a rare heart infection) is usually caused by certain strains of adenovirus. Finally, I report an outbreak of serotype 7 that caused a serious outbreak in 2014 with 136 (69 percent) of 198 persons with adenovirus-positive respiratory tract specimens were hospitalized, out of which 18 percent required mechanical ventilation, and 5 patients died (“Human Adenovirus Associated with Severe Respiratory Infection, Oregon, USA, 2013-2014”, Emerg Infect Dis. 2016)
After I finish a 17 year-old WCC and sports physical, my attending grabs me to come take a listen to 9-month-old twins with bronchiolitis. “Could my medical student listen?” she asks the parents. These are the sickest patients I’ve seen today and show classic signs of adenovirus: conjunctivitis, runny nose, cough and pharyngitis. I listen to their lungs and hear inspiratory crackles with an expiratory wheeze. There are no signs of dehydration, such as lack of tears while crying, poor capillary refill, poor urine output. They are not in respiratory distress, e.g., nose flaring, intercostal retractions, abdominal muscle use. We sent the family home with instructions regarding what would merit a follow-up visit.
I’m learning that most of a pediatrician’s job is educating parents on the basics: when to brush teeth, how often to breastfeed, what car seat should the child be in, how much should the baby drink, when to stop using the bottle. The format of a well child check is standardized for each age. Despite the hundreds of millions of dollars spent to install Epic, it doesn’t default to the practice’s preferred form for, e.g., a 10-year-old, when a 10-year-old patient is being seen. The efficient physician populates a custom-made SmartText for a 10 year old, and then fills out certain milestones that were filled out by the parents on paper.
Statistics for the week… Study: 5 hours. Sleep: 8 hours/night; Fun: 1 night. Example fun: best friend from college visits this weekend. He is an M3 at a different school who has already been on rotations for six months: “Third year sucks. Physicians claim that they remember third year as the best. Bullshit. It is mostly waiting around doing nothing, and yet you have no free time.” He adds: “Scary to think this is all the training we have in some areas. For example, if you don’t want to be a surgeon, you will be a practicing physician with only a few weeks of surgery experience. It wouldn’t surprise me if some physicians don’t even know how to start an IV anymore.” He is looking forward to psychiatry: “You talk to each patient for 30 minutes, chart a note during the interview. Pay for psychiatrists grew 15 percent last year. If this continues for 5 years, a psychiatrist will get paid as much as an orthopedist and get out every day at 2:00 pm.”
The rest of the book: http://fifthchance.com/MedicalSchool2020
Full post, including comments