Compare estimates of white male economic importance from TV viewers, streamers, and readers?
I often ask folks outside of Florida whose primary source of news is from New York-based media for their estimate of how often a typical house in coastal South Florida is hit by a major hurricane. The estimates range from between 1 and 5 years. (The historical prevalence if more like every 50+ years; Palm Beach County was last hit in 1949 and Tampa has gone more than 100 years (since 1921).)
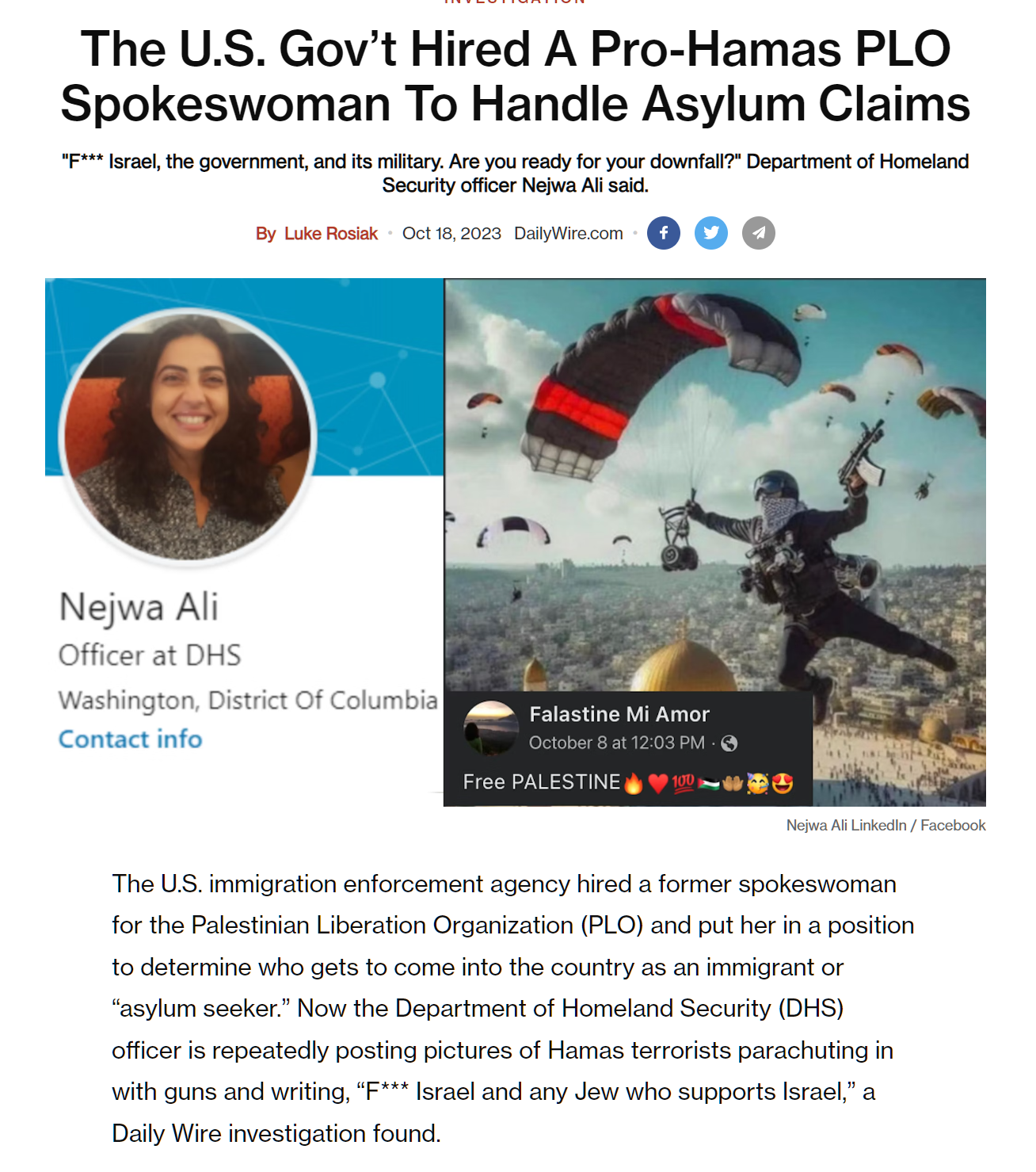
While watching an NCAA Final Four game with our local basketball fans I observed almost no white males in the commercials. There was an occasional white female with a Black sex partner (spouse or “date”). There was an NCAA house ad in which a fictitious college classroom was presented and there were a few white male students learning from the wise (Black) professor. The overwhelming number of people presented as business executives or valuable consumers, however, appeared to be either Black or Hispanic. A viewer might easily imagine that a restaurant, for example, would be able to prosper without any white male customers and, certainly, any business could be run without any white male employees.
I wonder if this suggests a good subject for a sociology or social psychology master’s thesis:
Compare the estimates of white male economic importance in the U.S. made by the following groups of people: (1) those who watch broadcast TV with commercials, (2) those who watch streaming services such as Netflix, and (3) those who neither watch TV nor stream (all four of them in the U.S. who actually read books?).
What actually is the importance of non-Hispanic white males in the U.S.? ChatGPT says that white males are 30% of population, pay 37-40% of all federal receipts, and receive only 10-15% of welfare. In other words, they’re perfect “tax cattle”. How about in driving the S&P 500’s apparently unstoppable rise? ChatGPT says white males are 72 percent of Fortune 500 senior executives, which is inconsistent with its earlier estimate of “37-40% of federal receipts” because Fortune 500 execs are rich and the top 1% of Americans alone pay 40% of federal individual income taxes. Maybe white males pay 80% of federal income tax and then a more equal share of other taxes, such as Social Security? Income tax is about half of federal revenue. A better estimate might be 60% of federal receipts.
(What about white women who do appear in the TV commercials that I saw, but at low levels of representation? ChatGPT says “as a group, women almost certainly receive more in government benefits than they pay in taxes, especially if you include benefits tied to children” (the “single mom” cheat code for 18+ years of taxpayer-funded life) and “White women, as a group, likely receive slightly more in government benefits than they pay in taxes over their lifetimes—but they are much closer to balance than women overall.”)
Related…
Some examples of a white-male-free U.S.: