Some data nerds at University of Washington, specifically within the Institute for Health Metrics and Evaluation, have prepared a state-by-state forecast of coronaplague peak and hospital bed/ICU demand/shortage. (See previous post: “Will New York run out of hospital beds?”)
They’re projecting roughly 80,000 deaths in the U.S. through August 4, 2020, with a range of 40,000 to 160,000. In other words, about as bad as four years of easily preventable deaths due to driving (assuming that half of driving-related deaths could be prevented with improved infrastructure and technology). The peak will be April 14, 2020, just in time for taxes. We will need roughly 1.2X as many ICU beds as we had before any ramp-up (shortfall of 14,000+ ICU beds divided by about 80,000 total ICU beds in 2018). We need only about 19,000 ventilators nationwide (this is completely inconsistent with New York Governor Cuomo’s statement that his state alone needs 30,000; the “experts” say New York will need closer to 4,000 and, in a worst-case scenario, no more than 10,000 (this is a situation in which we should listen to politicians rather than “experts”?)).
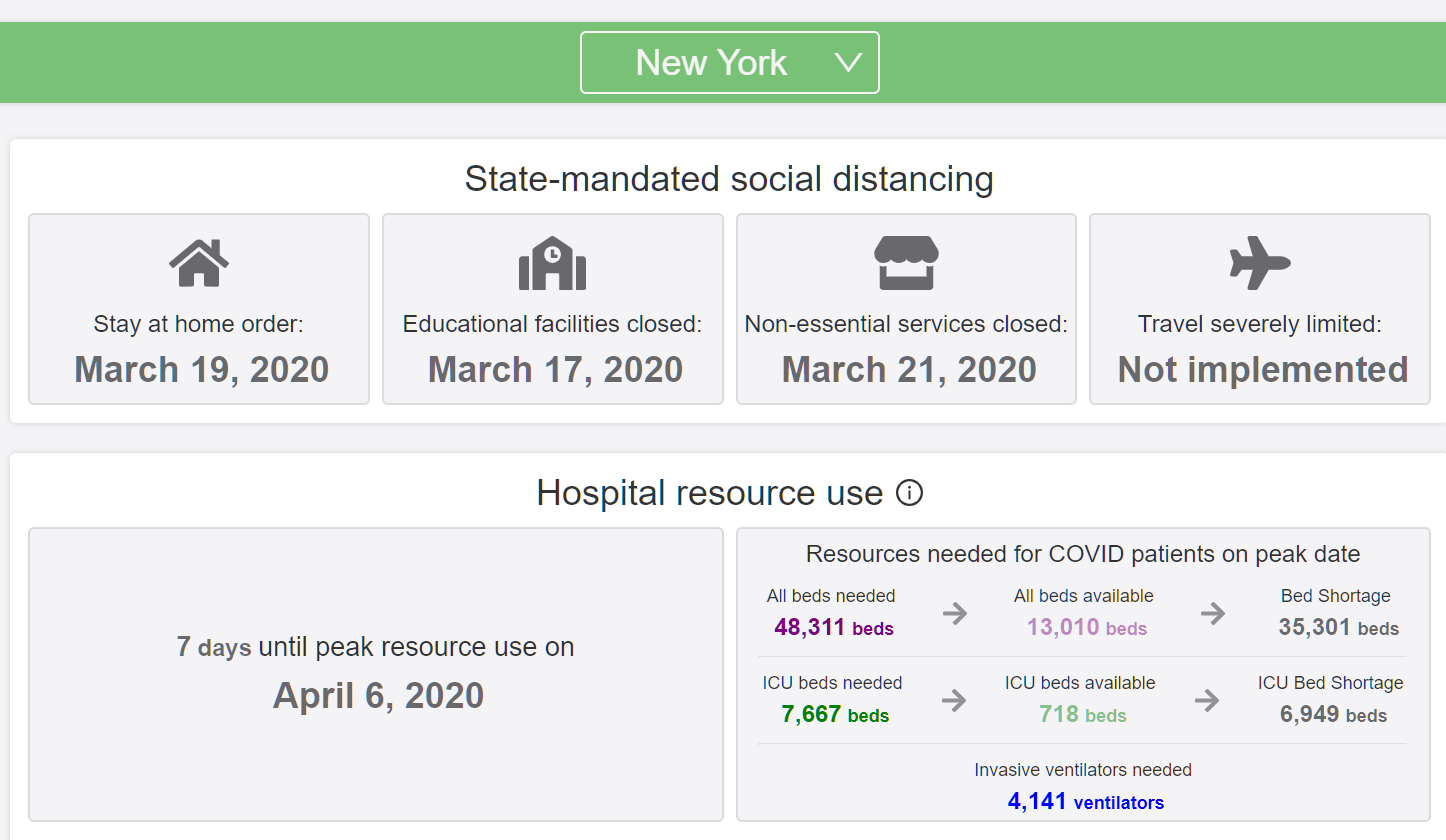
If you’re a New York elite, is it rational to limo out to Teterboro and get into a Gulfstream headed to Florida? Absolutely, says this model. New York has 13,000 hospital beds available and will need 48,000+ on April 6, 2020. The state has 10% of the available ICU beds that it needs. 1/8th of the Americans who are going to die from COVID-19 live in New York (which contains roughly 1/17th of the U.S. population) and presumably the majority of these will be from New York City.
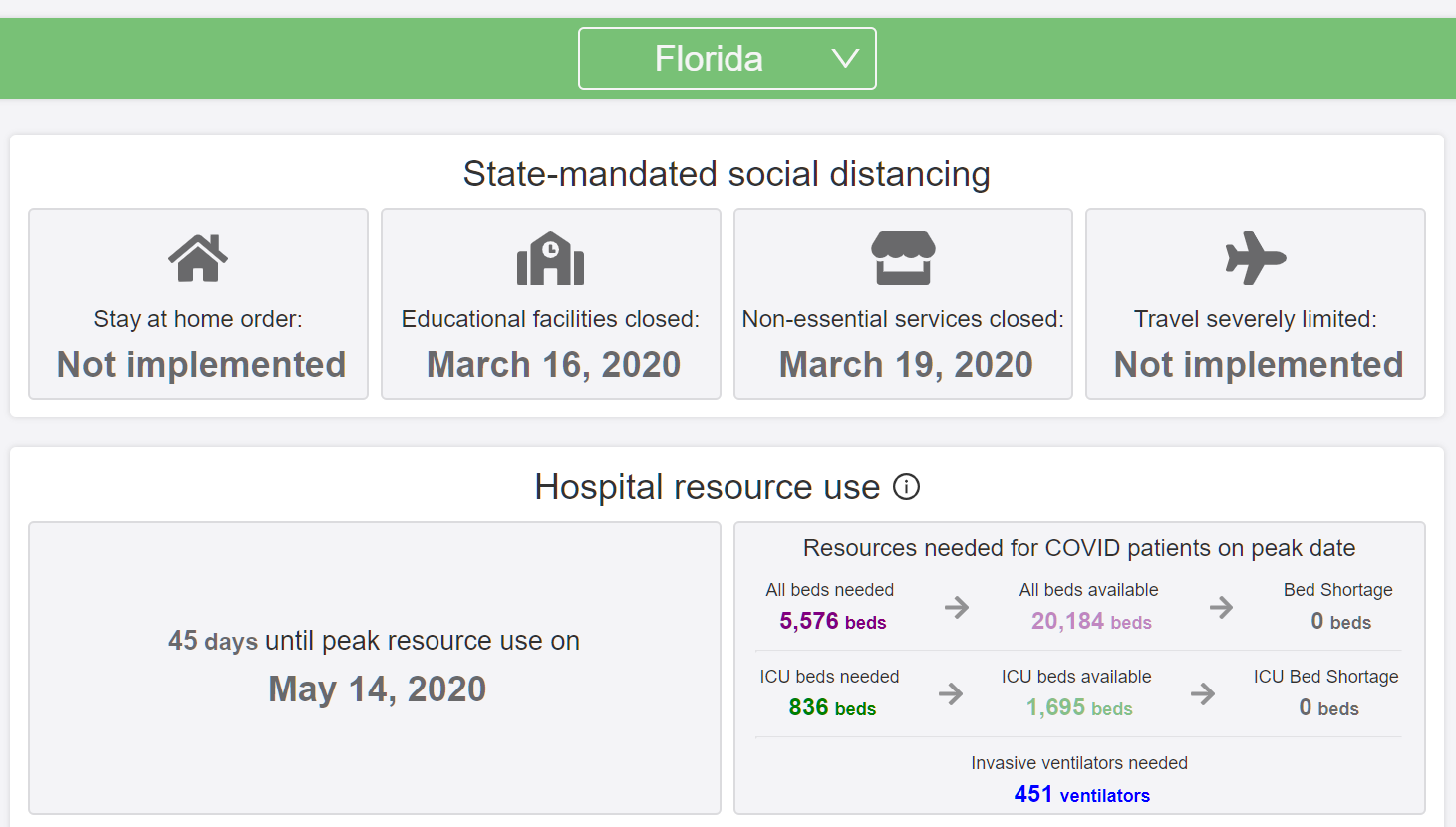
What about Florida, whose tax burden is dramatically lower than New York’s (highest taxed state in the union). In this land of minimal government, they will have 4X as many hospital beds as they need, 2X as many ICU beds. Nobody in Florida is going to die from COVID-19 due to lack of health care availability. With a larger population than New York’s, Florida will suffer only about 3,300 COVID-19 deaths (not everyone can be saved, unfortunately, even with unlimited health care). The peak in Florida won’t come until May 14, 2020 (tough to square with exponential growth).
How about the second- and third-highest tax burden states in the union, Connecticut and New Jersey? Both will be disaster areas, project the data nerds, with demand for ICU beds being 5-7X the supply.
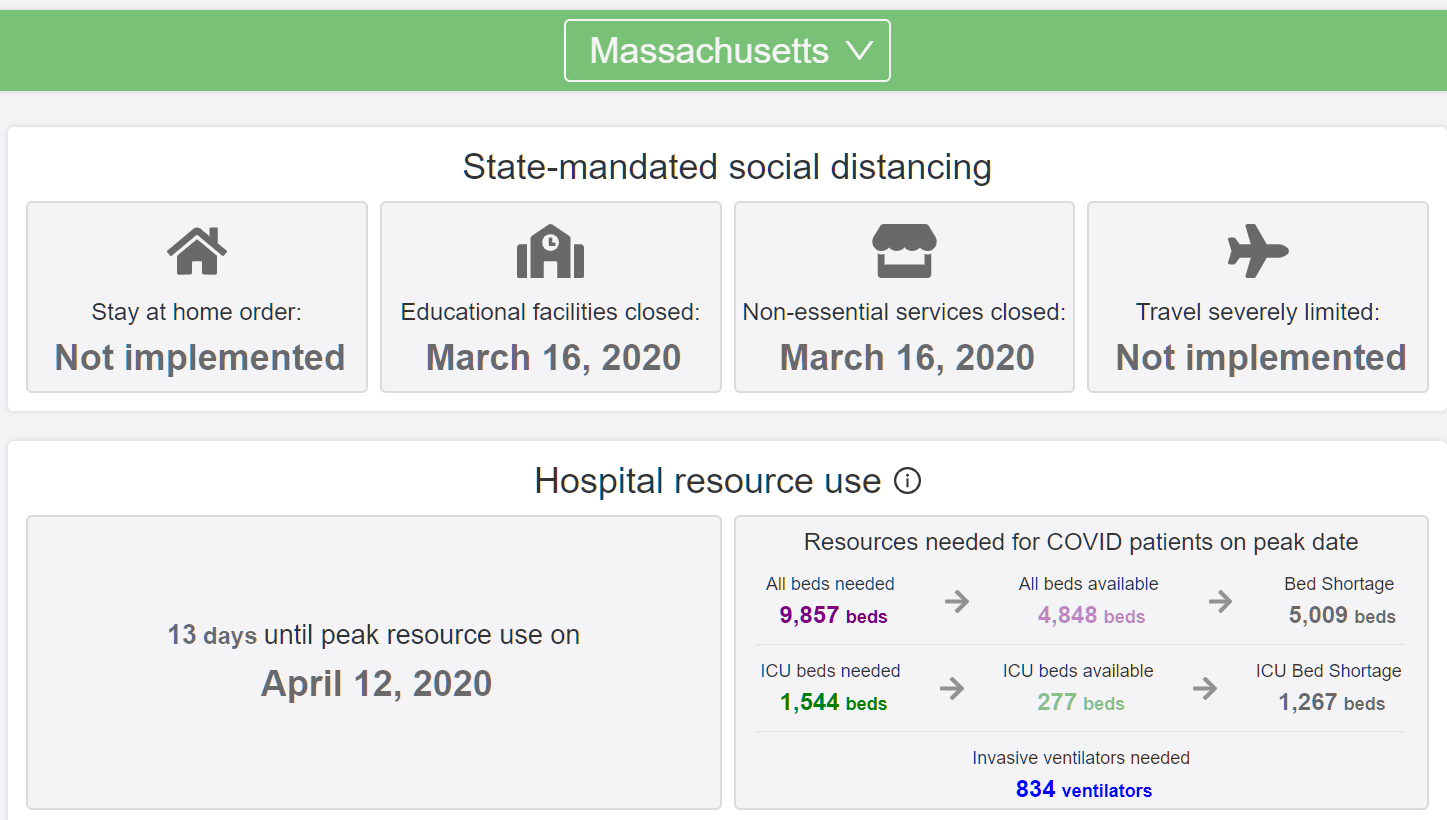
How about Massachusetts, where we pride ourselves on science-informed laws made by a legislature untainted by Republicans (the “science-denial party”)? Demand for beds will be 2X supply. Demand for ICU beds will be more than 5X the supply. Nearly as many people in Massachusetts will die as in Florida, despite that sun-drenched state having a much larger population.
An associated paper explains the model. What’s even worse than 80,000+ Americans biting the dust, many because their state’s government-directed health care system was pushed over by a slight breeze of excess demand?
State governments have cancelled elective procedures (and many hospitals but not all have followed suit). However, this decision has significant financial implications for health systems, as elective procedures are a major source of revenue for hospitals.
The biggest question mark for me is their forecast of ventilator usage (19,000 best-estimate for peak; 40,000 worst-case). If the data nerds are right, we have way more ventilators in the U.S. than we need to handle this challenge. We had at least 62,000 ventilators in service back in 2009 (source), plus another 100,000 older models in storage. Presumably a lot of the in-service ones are tied up with people who are sick with chronic conditions, but all of the older models should be available and that is a more than adequate resource. If these folks are right, everyone who is freaking out about ventilator supply is wrong.
Thanks for reading the paper. The forecasts are based on the assumption that all states will lock down before the end of this week:
They’re primarily worried about ICU beds and staffing (although IIRC they’re saying 25% more ICU beds are needed, not 50% more).
If lockdown happens everywhere before the end of this week, and if 25% more ICU beds can be provided and staffed, they’re forecasting 80,000 deaths. If not, the number of deaths will be higher, because not everyone who needs intensive care will get it.
They’re also assuming adequate personal protective equipment is available. If that’s not true, health-care workers will get infected, reducing capacity further as people get sick (and die). If the team’s forecast of ventilator demand is correct, and if the federal government can arrange to get ventilators to states which need them, then ramping up PPE manufacturing (like masks and gowns) seems like it should be a higher priority than ventilator manufacturing.
The top-level page says we need 34,754 ICU beds on April 14, 2020 and that there will be a shortage of 14,601. From this I infer that we will have 20,000 COVID patients in ICU beds and 14,601 on some kind of second-rate care. So I guess you could say that we need 1.7X spare ICU beds over a baseline of empty ICU beds. But the U.S. had about 80,000 ICU beds in 2018. https://www.aha.org/statistics/fast-facts-us-hospitals . So actually we need to boost total ICU beds in the U.S. by only about 18%. Let me tweak the original post.
Here’s the high-level discussion of forecast excess demand, from the paper.
Hopefully you’re correct in saying that there should be plenty of ventilators to go around. The national stockpile alone has 16,000 ventilators.
On ventilators, a NYT article cites the following figure:
It’d be useful to see the actual report, and the model that this estimate is based on. But that doesn’t sound good.
Russil: I am shocked to learn that going from design to implementation under government supervision did not proceed efficiently or quickly! When you consider https://en.wikipedia.org/wiki/Lockheed_Martin_F-35_Lightning_II (begin in 1993, sort of operational by 2015) and https://www.nbcnews.com/think/opinion/navy-spent-30b-16-years-fight-iran-littoral-combat-ship-ncna1031806 , how is it possible that the ventilator program went off the rails?
I was curious about the relatively low forecast for Florida. I know there seemed to be a delay in people taking it seriously, and there’s a lot of older retired people in Florida (which is why there’s so many hospital beds). Looking at the forecast data in the attached CSV, the model is forecasting about 500 hospitalizations in Florida by March 27 (which is where it was), with a doubling time of six days: 1000 by April 2, 2000 by April 10, after which it slows down further.
The Massachusetts data doesn’t match actual numbers so far. The model is forecasting 1860 hospitalizations by March 27; the actual number on March 27 was 288. So Massachusetts is doing a lot better than the forecast.
I hope that the research team can update the model and the forecasts as the actual number of deaths in each state increases. The actual effectiveness of social distancing measures may vary across states.
It is always a shame to ruin a beautiful model with actual data! That’s what folks who are “anti-science” like to do.
As noted in the paper, the model is based on the number of deaths in each state. Compared to the number of confirmed cases, the death count is less likely to depend on the extent of testing.
You may be interested in this Washington Post article on coronavirus trutherism. Coronavirus modelers factor in new public health risk: Accusations their work is a hoax.
How can anyone doubt the modelers? Dr. Fauci on March 11: “The flu has a mortality rate of 0.1 percent. This has a mortality rate of 10 times that. That’s the reason I want to emphasize we have to stay ahead of the game in preventing this,” he added. https://thehill.com/changing-america/well-being/prevention-cures/487086-coronavirus-10-times-more-lethal-than-seasonal (i.e., 1% of those infected with coronavirus will die)
Today he is saying it will be closer to 100,000, 0.03% of the U.S. population of 330 million. These numbers are consistent if no more than 3% of Americans ever become infected. https://time.com/5812149/fauci-coronavirus-deaths-100000/
In other words, he is now expected the total deaths in the U.S. to be less than a European flu season (kills over 200,000, according to https://www.ecdc.europa.eu/en/publications-data/summary-influenza-2016-2017-season-europe ) and the death rate per capita to be lower as well (the EU has just over 500 million people, which is why they desperately need low-skill migrants!).
If Dr. Fauci revises his estimate downward just one more time, two years of COVID-19 will kill fewer Americans than a month or two of medical errors. https://www.npr.org/sections/health-shots/2016/05/03/476636183/death-certificates-undercount-toll-of-medical-errors (250,000 per year).
Another example of coronavirus skepticism, from someone who’s much more reputable than Shiva Ayyadurai: renowned legal scholar Richard Epstein. Isaac Chotiner at the New Yorker did a long and remarkably contentious interview: The Contrarian Coronavirus Theory that Informed the Trump Administration. You may find Epstein’s essay interesting. It suffers from being published two weeks ago: initially he predicted that the number of deaths in the US might rise eight-fold, from 67 to 500 or so. Since then he’s revised his prediction to 5000 deaths. (My own prediction is that the US will pass 5000 deaths by April 2, and 10,000 deaths by April 6.)
What about location, location, location? If for example all of Florida’s ICU beds are in the Panhandle (they are not) but most of the cases are from Ft. Lauderdale down to Key West, that is a problem.
You’ve heard the old saying?
“All models are wrong. Some models are useful. “
I believe that rough quote is attributable to George Box
“These numbers are consistent if no more than 3% of Americans ever become infected.”
Correct. Given the contagiousness of the virus, this requires extraordinarily expensive measures (“suppression”), which is what we’ve been arguing about. Fauci’s estimate is consistent with the University of Washington estimate (roughly 80,000 deaths). Again, this estimate is based on the following assumption, which shuts down a big chunk of the economy:
Saying “look, this only kills 100,000 people – why do we need these hugely expensive measures?” is overlooking the fact that the 100,000 estimate is assuming the hugely expensive measures.
With less expensive measures (“mitigation” instead of “suppression”), the point of the Imperial College paper is that the demand for intensive care far surpasses the available capacity. This results in a death rate higher than 1%. In the initial Wuhan outbreak, when the health system was completely overwhelmed, the death rate was 5.8%.
A ballpark estimate: suppose that “mitigation” limits the infection to 20% of the population, or about 60 million people. With a fatality rate of 1%, that’s 600,000 dead. Say that 5% of cases require intensive care, and roughly 60% of those don’t receive it because the health system is overwhelmed. That’s about another 2 million dead. Total, about 2.5 million dead (death rate 4%).
Does that seem like an unreasonable estimate?
So Angela Merkel told Germans that 70 percent of them would be infected, but our state governors’ school closures and other measures will keep the U.S. infection rate to 3 percent and therefore Dr. Fauci is not contradicting himself by saying that coronavirus will now be far less deadly than baseline U.S. medical errors?
You didn’t answer my last question!
Merkel’s warning (on March 11) that up to 70% of Germans could be infected would have been based on the assumption of no public health measures at all. If a new virus with R0=3 spreads within a population with no immunity, you get a 67% infection rate.
None of your estimates make sense to me. If the population has no immunity and the disease cannot be eradicated, eventually 70 percent of people will get it. That’s what Merkel was saying. With school closures and other social distancing measures it might be possible to delay the point at which infection reaches 70 percent, but you’re not going to change the endpoint.
Here’s a Harvard School of Public Health professor. He is saying 40-70% of the worldwide population will be infected. He doesn’t say “Oh, close the schools for three weeks and shut down some of the stores and you can cut that to 3%”. https://www.cbsnews.com/news/coronavirus-infection-outbreak-worldwide-virus-expert-warning-today-2020-03-02/
“Here’s a Harvard School of Public Health professor [Marc Lipsitch]. He is saying 40-70% of the worldwide population will be infected. He doesn’t say ‘Oh, close the schools for three weeks and shut down some of the stores and you can cut that to 3%’.”
That’s what the Imperial College report is saying. (Judging from his Twitter feed, Lipsitch regards it favorably.) Use suppression to keep the virus limited to a relatively low number of cases, until a vaccine is available to immunize the population, which could be 18 months or more.
South Korea demonstrates that it’s possible to contain the virus through widespread testing, contact tracing, and social distancing. (They’re at 10,000 confirmed cases out of a population of 50 million, or about 0.02%, and the number of new cases daily is less than the number of recoveries.) Of course the US is way past that stage.
Well, if you believe that the feeble and late actions of some governments will keep the infection rate to 3%, more power to you! Certainly that would surprise the Oxford team who think that roughly 50 percent were infected before the U.K. went into its non-locked-down lockdown.
The wise California government will ensure that the disease cannot spread there. They will move 6,000 people from individual tents to indoor concentration camps: https://www.lamag.com/citythinkblog/the-city-plans-to-move-6000-homeless-angelenos-into-l-a-rec-centers/
If you have 200 formerly homeless guys living together in a gym, there is no way that a cold, flu, or coronaplague could spread from 1 to the rest, right?
https://www.dailybreeze.com/2020/03/18/amid-coronavirus-concern-6000-beds-for-las-homeless-coming-to-parks-facilities/ has a photo of the facility that will ensure no disease can spread from one inmate to another.
Speaking of inmates, the U.S. has 2 million in prison. That’s 0.6% of the population right there. How are they not all going to get a disease with an R0 of more than 3?
Seems like an argument for strengthening the effectiveness of public health measures, not an argument for inaction.
And again, the University of Washington forecasts (about 80,000 deaths nationwide) are assuming widespread and effective social distancing by April 5, and expansion of health capacity to meet the excess demand. The less effective public health measures are, and the less the health system is able to meet demand, the more deaths there will be.
This graph that shows the “bell curve” overtime https://aatishb.com/covidtrends/ is a fair indicator (if you accept the 2 countries’ data, China and South Korea) of when countries will start to see a peak and a drop on COVID-19.
It agrees with the theory that the people freaking out are the wealthy who don’t want patients coming to their neighborhoods. Haven’t been near any hospitals to look for signs of patients being directed away from wealthy neighborhoods, but neither has anyone else in the media.
“In Florida, the model predicts 465,699 people will be hospitalized because of COVID-19, the illness caused by complications from the virus, by April 24, but there will only be 36,384 hospital beds available by that date.”
Source: Miami Herald March 23 – “FL Gov. DeSantis Pushes Back Against Statewide Stay at Home Order”.
If you want to hear from someone who knows what their talking about watch the interview with the head of South Korea’s Pandemic Response Team https://video.search.yahoo.com/search/video?fr=crmas&p=asian+boss+south+korea+covid-19#id=31&vid=b2197205c1fbe790be8ea3291dcad9dd&action=click
Jack: thanks, that article is based on another model I hadn’t seen before (COVID Act Now), which also provides state-by-state forecasts. It doesn’t assume effective social distancing – instead, it provides forecasts for different social distancing scenarios.
In Massachusetts, the projection is that shelter-in-place with strict compliance will limit the infection to 4% of the population, with 3000 deaths. https://covidactnow.org/state/MA
I’m surprised that nobody has done a random sample within the U.S. population or at least within a U.S. metro area. If the Oxford epidemiologists are correct, Massachusetts already has an infection rate higher than 4% and will settle in at 50-70 percent soon enough. But since the only people who are tested are the hospitalized and we have no idea of the hospitalized/infected ratio, we have no idea if Massachusetts is 0.1, 1, 5, 10, 25, or 50 percent infected right now.
Sounds like people are working on serological testing. https://www.vox.com/2020/3/30/21186822/immunity-to-covid-19-test-coronavirus-rt-pcr-antibody
Russil: We have to make decisions on whether to restart the economy sooner than any new test will be available. We already have the PCR-style tests for the actual virus. Especially when we consider that a diagnosis of COVID-19 has no therapeutic value (since there are no effective treatments), why not dedicate 1% of our testing capability to a population-wide study?
Turns out Iceland has been doing randomized tests! Based on results so far, about 6% of the population is infected. About half of those infected are asymptomatic. https://fortune.com/2020/03/27/coronavirus-testing-us-iceland-cdc-trump-decode-covid-19-tests/
Also, Noah Smith summarizes an AEI roadmap for restarting the economy: https://www.bloomberg.com/amp/opinion/articles/2020-03-30/a-smart-plan-to-end-the-u-s-lockdown-arrives-just-in-time
Russil Wvong – Are you guys tracking the accuracy of this at all? I’ve only watched for California, but it looks like the actuals for Mar 27,28,29 are much lower than the predictions made based on the Mar 24 data. It also looks like the predictions for Mar 30 and onward, based on the Mar 29 data, look the same as those based on the Mar 24 data, just delayed by the 3 days.
Alan: I haven’t been following the California numbers. Since I’m in Vancouver, I’m mostly worried about the Washington state numbers.
Sorry, I assumed from your “Thanks for reading the paper” comment that you were associated with it in someway.
No worries! I said “Thanks for reading the paper” because I had included a link to it in a comment on a previous post.
In general hospitals aren’t owned by the state, most are private, some non-profit, and a few public. So taxes should have practically no effect on number of beds. Considering that roughly 25% of medical spending goes to the last year of someones life Why would anyone be surprised that FL, with its loads and loads of retirees has hospital systems that turns that into more beds? I’d be shocked if they didn’t have the most beds per capita.