Book about a serial killer that is important for both pro-vaxxers and anti-vaxxers
I recently finished listening to American Predator: The Hunt for the Most Meticulous Serial Killer of the 21st Century, a book about Israel Keyes. Mr. Keyes was born at home, one of 10 children, and was not only never vaccinated but didn’t interact with medical doctors for his first 18 years. He never even had a birth certificate. (The events of the book occur before the Sacrament of Fauci became available and, therefore, “never vaccinated” refers to the pre-2020 standard childhood vaccines.) From the perspective of those who are pro-vaccination, the fact that Mr. Keyes became a serial killer will be important (i.e., without the 57 shots recommended by the CDC through age 18, Mr. Keyes’s mental health was impaired, though the book describes him as “bisexual” and membership in the 2SLGBTQQIA+ community is considered a sign of superior mental health, so maybe being Bi and being a serial killer cancel out?). From the perspective of those who are anti-vaccination, Mr. Keyes being extraordinarily robust, intelligent, and conscientious will be important (of course, he eventually makes one mistake that leads to his arrest).
According to the author, we didn’t learn as much as we could have about Mr. Keyes’s life of violent unprovoked crime due to the incompetence of the U.S. Attorney in Anchorage, Alaska, Kevin Feldis (now a partner at Perkins Coie). He allegedly refused to allow the FBI professionals interrogate the suspect and, instead, inserted himself.
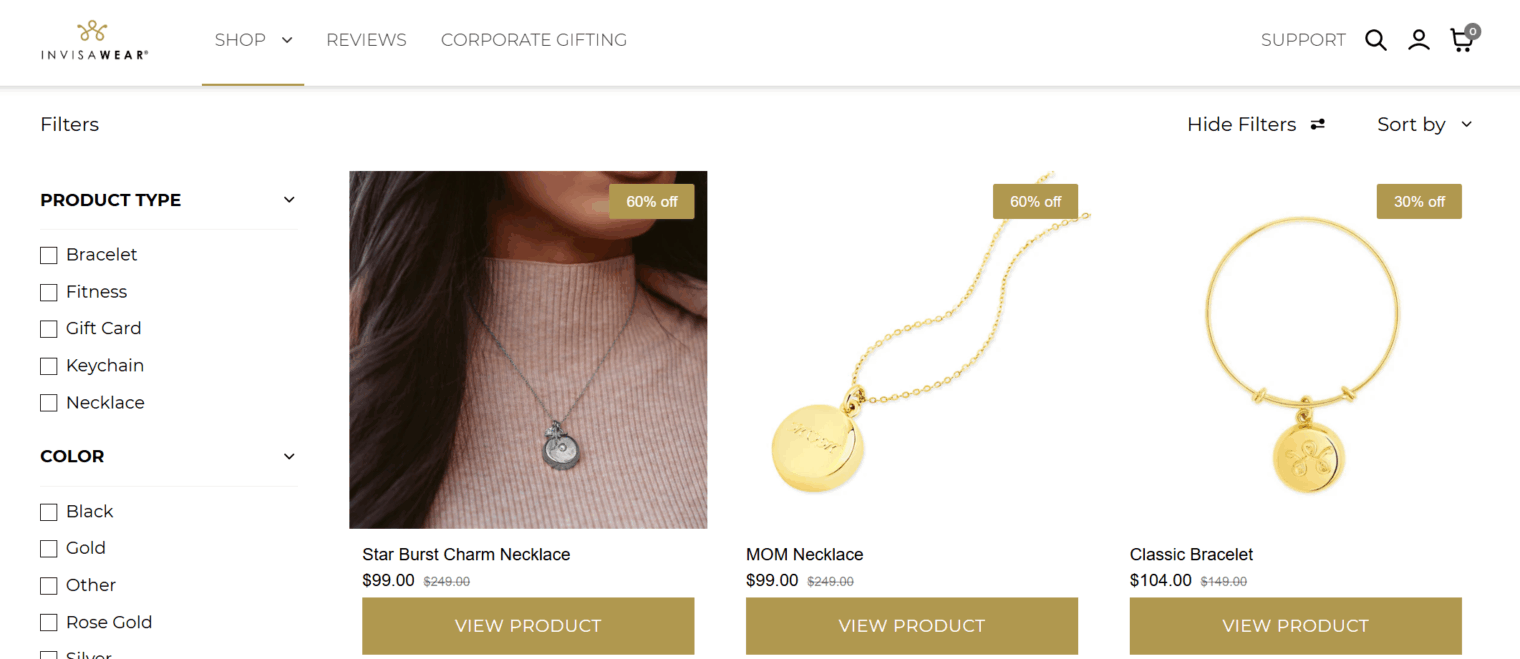
The book might inspire you to develop or purchase a “panic ring” that can be pressed one-handed to summon the police. Keyes was usually able to tie up his victims before they were able to make any phone calls, but they generally would have had enough time to move a thumb on top of a forefinger ring. If the GPS location and mobile data connectivity services are handled by a Bluetooth-linked mobile phone, the ring shouldn’t need to be large even with a long battery life. It looks as though a phone-linked necklace/bracelet is available from invisaWear:
The victims weren’t immediately gagged so perhaps it would also work if the phone were just constantly listening for “I have an itch” or a similar phrase. If Hitler 2.0 can get Neuralink to work, perhaps it would be sufficient just to think “I need to be rescued”.
Full post, including comments