Why haven’t name-brand hybrid e-bikes gotten dramatically lighter?
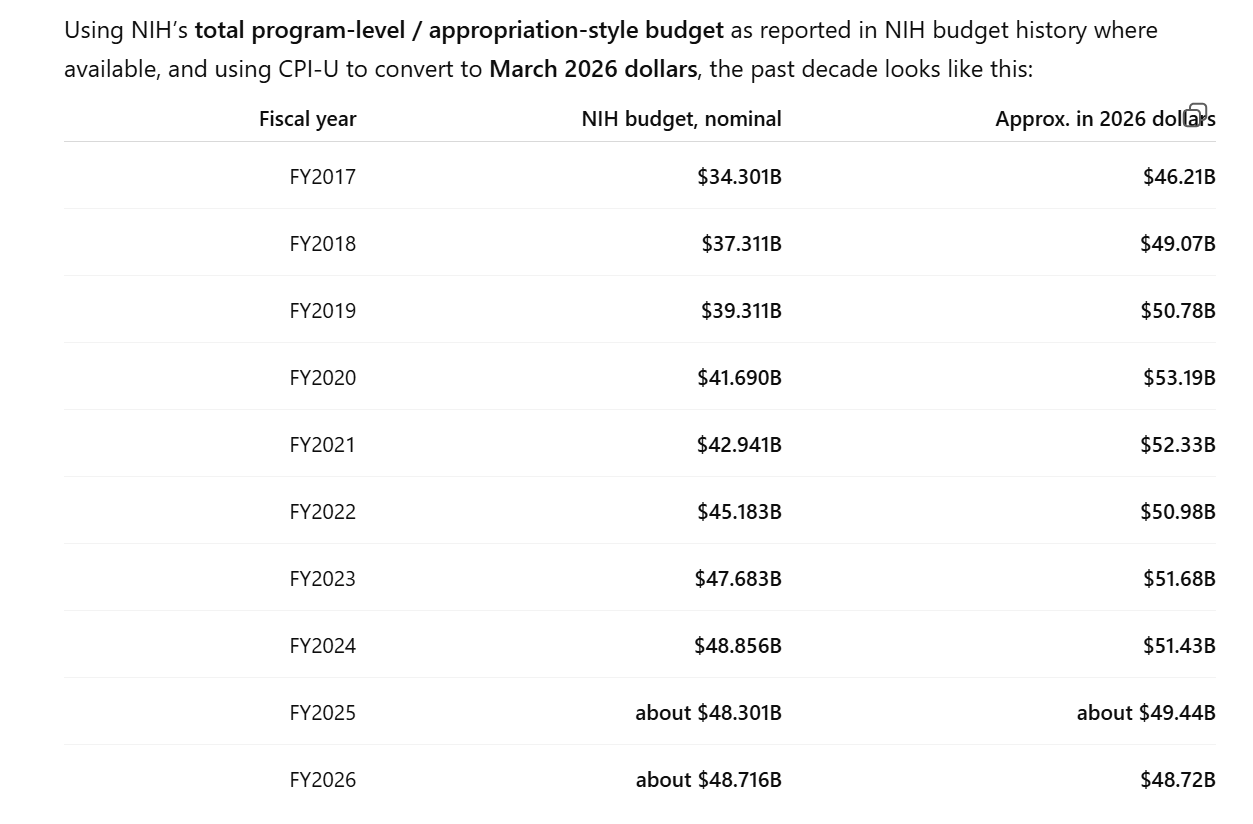
Summer is here for most of those who escaped the New England lockdowns during coronapanic. Average Nashville high temp for May is 79 degrees (unlike Maskachusetts, Tennessee has no state income tax and no estate (death) tax; state tax competitiveness index).
Many moons ago, I wrote about a 2013 Trek e-bike that weighed 52 lbs.: Trek T80+ Electric Bike Review. The ungainly unbalanced rear hub motor beast has a 250W motor and a 250 Wh battery. I bought it as an experiment and figured that if I loved e-biking I would treat myself to a fancier mid-drive one when the Trek died. Here we are 11 years after the closeout purchase and the Trek has not died. It’s on its second chain and has needed a new rear tire, but otherwise just works. The range is more than adequate for running errands around Jupiter and bike theft is a minimal issue (if the Florida police do catch a bike thief do they say “Where did you think you were, San Francisco?”; I sometimes use the built-in wheel lock if leaving the bike for an hour or two). The ancient Trek has the “torque sensor” that is advertised as a selling feature in 2026 by e-bike vendors, though the company (BionX, in the Islamic Republic of Canada) that made the electric gear went belly-up in 2018.
I’d love to buy a new e-bike if I could find the same comfortable geometry and the same motor/battery power at 33 lbs. Is that possible? (TL;DR: nobody has ever managed to make mid-drive light; mid-drive was the Holy Grail 10+ years ago, but it might be an emperor with no clothes except for climbing steep hills (certainly the old Trek’s hub motor was fine for climbing hills in Eastern MA)) For reference, let’s have a look at the upright riding position of the ancient Trek:
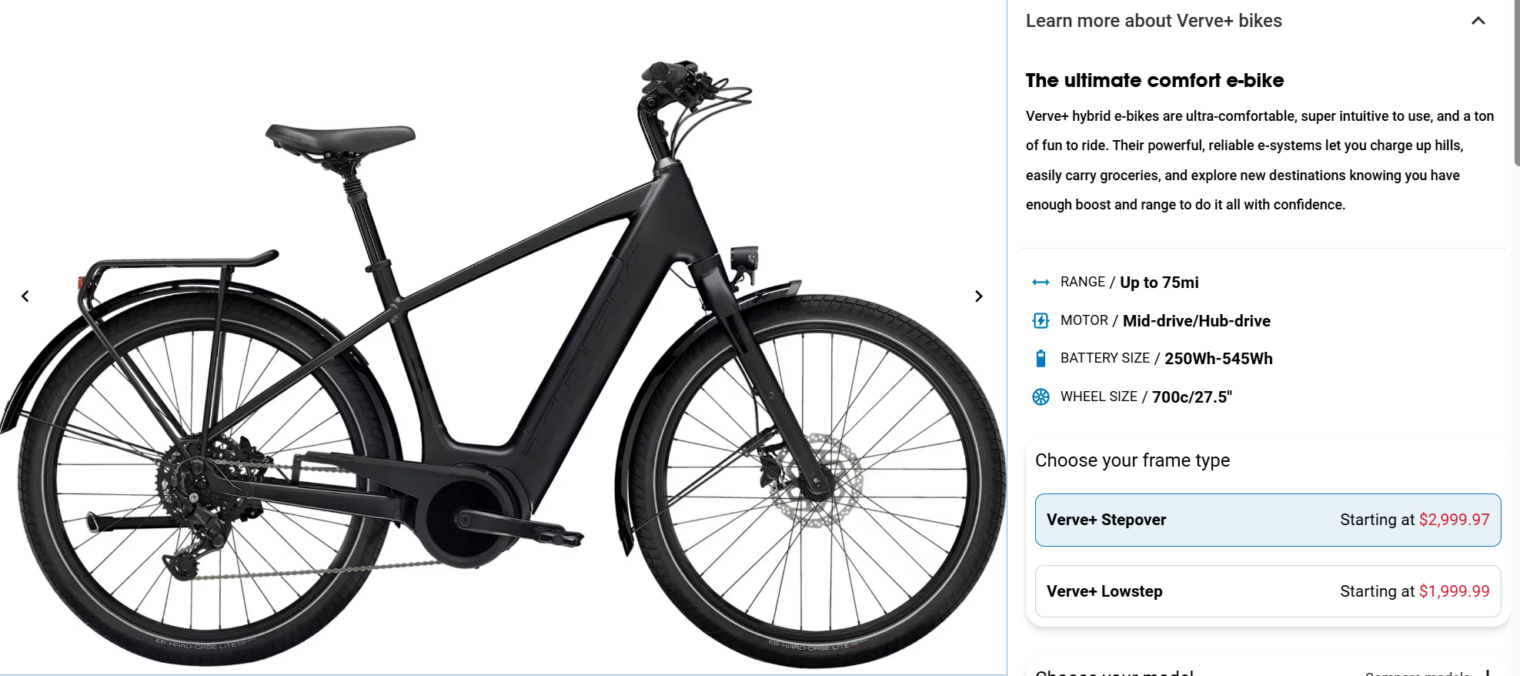
How much progress has there been in this industry? The closest Trek current bike that I can find to the T80+ is the Verve+, starting at $2,000. The versions that are the most popular would weigh about 65 lbs. in a larger frame size.
The cheapest lightest version of this bike has the same motor/battery specs as my “survivor”. It is spec’d at about 42 lbs., but that’s for the M size and mine is an XL so let’s say that it would be 44 lbs. in L or XL. That’s not a negligible reduction, but the T80+ was literally thrown together and it is way off my 33 lb. spec.
What if we spent $6,749 on a Cannondale FlyingV (plus a $15 E-bike Battery Recycling fee?!?). The web page includes the word “weight” in numerous places to crow about how light the bike is due to its carbon fiber construction. The one spec they left out, though… the weight. It’s got 600 watts of motor power for people who want to kill themselves at 28 mph and 400 Wh of battery. An independent review says it weighs 40 lbs and it doesn’t have the suspension seatpost of the old Trek T80+. The review makes it sound uncomfortable as well: “The riding position aboard the FlyingV is balanced, fairly upright but with a sporty edge. The stance suits the bike’s character to a tee. If you want to fly, you’ll need to be at least a little fit and flexible – this isn’t your living room sofa on two wheels.”
Maybe the answer is a comfortable upright bike has to be super heavy? Giant’s $700-900 “city” bikes weigh 25-30 lbs., a fair amount more than a $1,000 non-electric road bike at 20 lbs. (examples). When road bikes are electrified they don’t get that much heavier. Here’s a road bike with the same 250W/250Wh spec as the old T80+. The Ride1Up weighs 28 lbs., presumably in a medium size, and costs $2200 (almost the same as the $2100 2013 price of the T80+, which is $3000 today if adjusted for the inflation that the government tells us does not exist). The same company makes a more upright city-style bike that costs $1400 and porks out to 40 lbs. with a 360 Wh battery. What if you spend $7000 on a carbon fiber hybrid from Specialized, the Turbo Vado SL 2 6.0 EQ Carbon? It weighs… 40.5 lbs. and has 520 Wh of power.
How are consumers getting these monster bikes onto roof racks or even into the backs of their monster SUVs when it is time to take the bike in for service? It seems as though the bikes that are actually selling in quantity weigh 50 lbs. or more. A review of what Bicycling says is the sweet spot e-bike, the Aventon Level 3, doesn’t even mention weight. Nor is the weight found on the page that sells the bike. Gemini says the beast weighs 67 lbs. and “The [733 Wh] battery is removable, allowing you to reduce the total weight to roughly 58 lbs for easier transport.”
Did everyone get rid of their roof racks and replace them with hitch racks, some of which can hold bikes up to 80 lbs.? Save the planet by attaching it to a Tesla Y’s receiver hitch, but leave half the e-biking family at home because it says “designed to support vertical loads of up to 160 pounds”? The two-bike hitch racks empty can weigh over 50 lbs.; the four-bike ones weigh over 70 lbs.!); maybe better to buy a cheaper one from Torklift that can handle more weight (the same company sells a Toyota Sienna receiver hitch that can handle 700 lbs. of tongue weight, which might translate to 350 lbs. of e-bikes). If you search for “bent receiver hitch with bike rack” the Google returns stories from people who bent the hitch or, worse, the frame of their vehicle, by loading up bikes.
Circling back to my original question… why no 33 lb. comfy hybrid e-bikes given all of the progress that has been made in materials? ChatGPT says a 250 Wh battery weighs only 3-4 lbs. ChatGPT says that the killer is the motor: “A 250W mid-drive (bottom bracket) motor system typically adds ~6–10 lbs (2.7–4.5 kg) compared to a normal bottom bracket. … Ultra-light e-bikes (like Fiido Air) avoid mid-drives. They use small rear hub motors instead. That saves ~5–8 lbs immediately.” (apparently the feel and balance of the mid-drive is worth the extra weight for most consumers, but the “sweet spot” is “Lightweight hub motor + torque sensor”) ChatGPT says that 67 percent of e-bikes globally are sold with hub motors, not the mid-drives that I thought were going to dominate the industry. In Europe and for premium bikes, though, mid-drives are dominant. The mid-drives up wearing out the drivetrain, though, so the super heavy bike has to get loaded into the car for the trip to the bike shop more frequently… (see above)
ChatGPT says that Fazua, a Bavarian company founded in 2013 and now owned by Porsche, is the leader in making a lightweight mid-drive system. Their completed city bikes, however, weigh at least 40 lbs. Internet reviews of Fazua’s reliability are mixed, to say the least, compared to the standard Bosch. ChatGPT: “In general, Hub motors are more reliable than mid-drives”. So maybe the answer is that I can have a better balanced bike if the battery is moved to the downtube, but the architecture of the motor in the rear wheel needs to be retained in order to avoid what ChatGPT claims is a 5-8 lb. weight hit and a lifetime of additional maintenance.
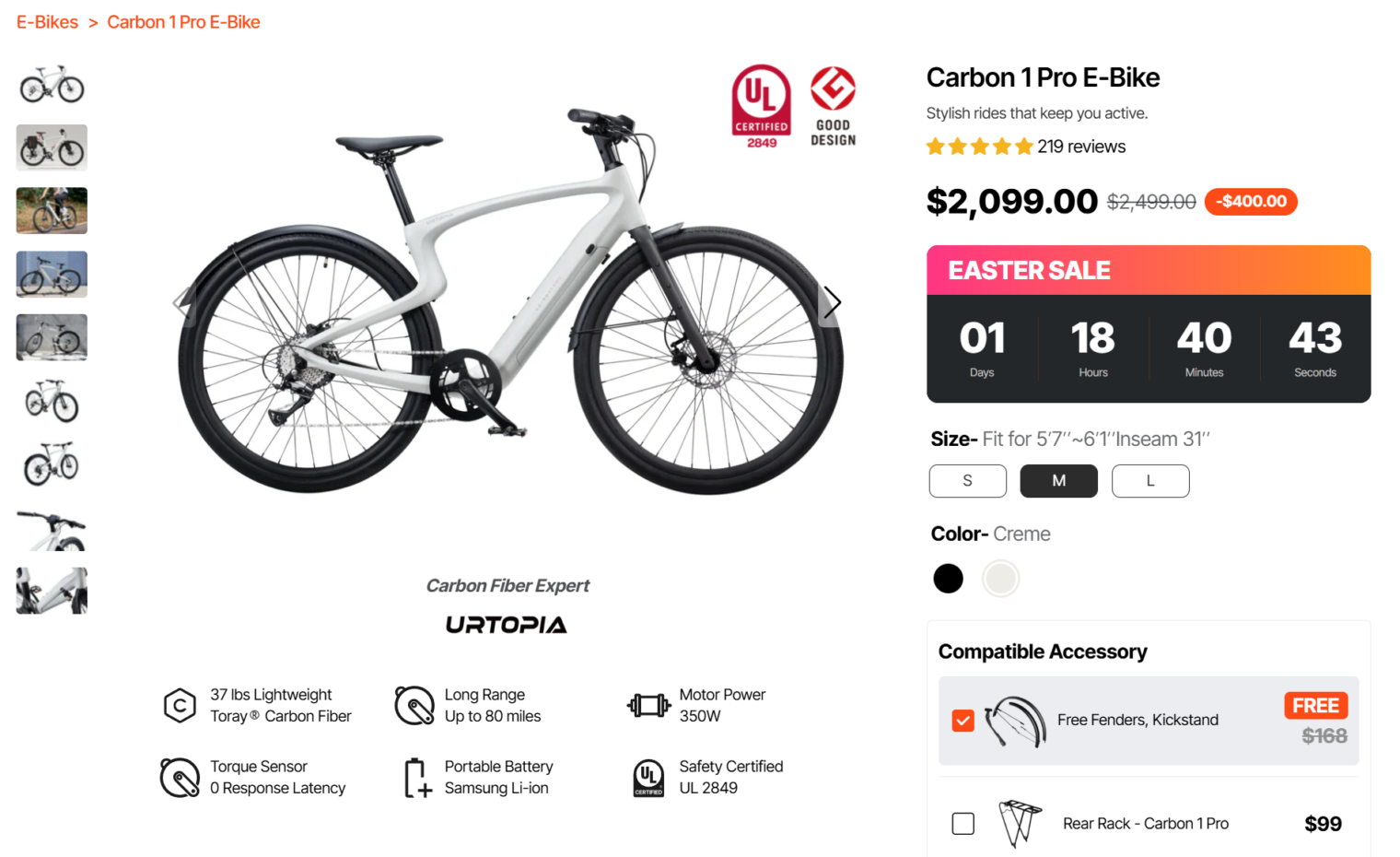
Let’s close with a bike that isn’t exactly “name-brand” (Giant, Trek, et al.), but that does seem to have the architecture that ChatGPT recommends… Urtopia Carbon 1 Pro (about $2100 as of a couple months ago). It seems to have a similar geometry to the $6,749 (plus $15 recycling/virtue fee) Cannondale, above. It lacks the suspension seat post of the old Trek, but maybe the flexible carbon frame absorbs shock reasonably well. Instead of cutting the promised-by-ChatGPT 5-8 lbs. by switching to a hub motor, the practical weight savings is only 3 lbs. (37 lbs. vs. 40). This one might be worth a test-ride (the company has dealers).
Full post, including comments