If you’re looking for a new book to read that provides some historical context for current events, The Siege (Ben Macintyre, 2024) might be a reasonable choice. It’s about a spring 1980 takeover of the Iranian embassy in London. Why did an Iranian Arab (more on that below) and his Palestinian friends decide that was rational to take hostages?
The plan was undoubtedly risky, but terrorist hostage-taking could yield spectacular results, and there was a precedent. Five years earlier, the Venezuelan terrorist Ilich Ramírez Sánchez, known as Carlos the Jackal, led a group of pro-Palestinian militants, the Arm of the Arab Revolution, in an assault on a meeting of OPEC leaders in Vienna. They took more than sixty hostages and killed three people. Ramírez Sánchez threatened to kill a hostage every fifteen minutes unless the Austrian authorities read a communiqué on the radio and television networks every two hours. After complex negotiations and a two-day standoff, the authorities agreed to broadcast the terrorists’ statement, and allowed the gunmen to fly to sanctuary in Algeria and Libya, having secured a large ransom and global publicity for the Palestinian cause. All the terrorists and hostages walked away. The United Nations Convention on the Prevention and Punishment of Crimes Against Internationally Protected Persons subsequently forbade granting safe passage to anyone killing, kidnapping, or attacking a diplomatic official, but, in practice, governments were prepared to negotiate. The assault on the Iranian Embassy was directly modeled on the OPEC siege. For reasons both symbolic and practical, London was selected as the ideal target. Many Iranian Arabs held Britain responsible for their plight: the British government had supported the semi-independent sheikhdom of Arabistan before switching allegiance to Reza Shah in 1925. The group would pass unnoticed among London’s large Middle Eastern population. “British police are not armed,” the Fox assured Towfiq. “They will not attack you.” London was packed with journalists and other members of media organizations, domestic and international, who were not controlled by the government. News coverage would be huge. With his command of English, Towfiq would manage negotiations with the police and the press.
In other words, the West’s previous accommodation of hostage-takers led to additional hostage taking. (Towfiq and the Palestinians circa 1980 probably never imagined that hostage takers would become the most celebrated folks on Ivy League campuses, though!)
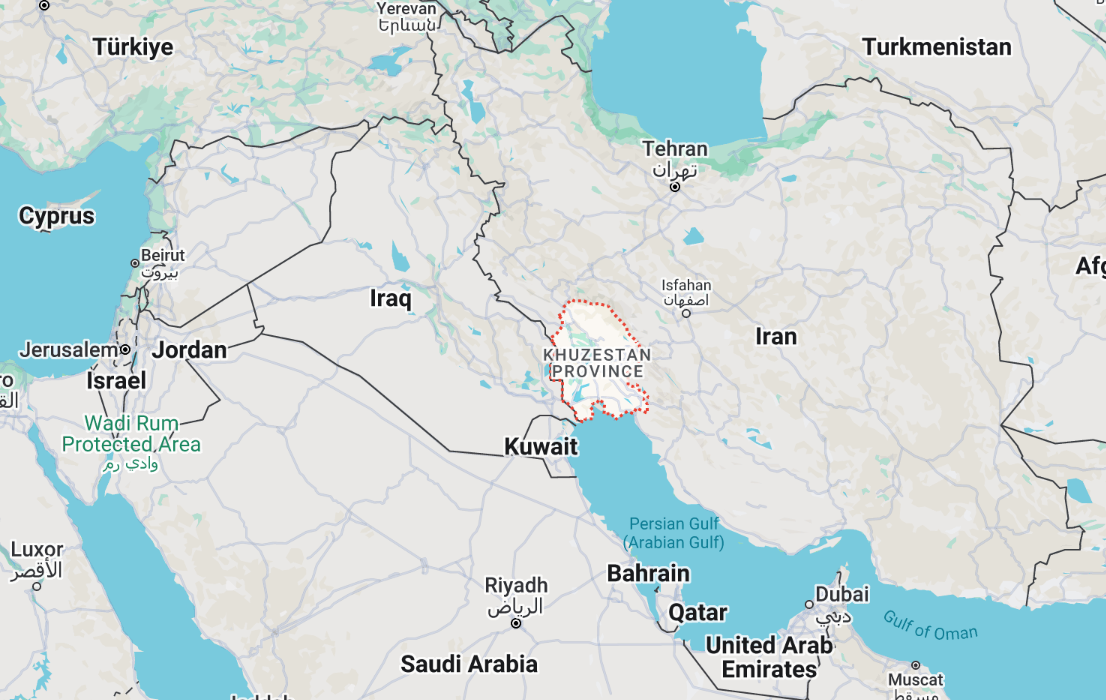
The root cause of the 1980 siege seems to be that much of Iran’s oil is underneath a part of a Iran that traditionally contained no Iranians.
The region abutting the Persian Gulf known to its Arab inhabitants as Arabistan, or Ahwaz (which is also the name of the region’s capital), was once the center of an ancient civilization. The majority of its inhabitants are Arabs, Shia Muslims, but they are ethnically distinct from the Aryans of Iran, or Persia, as it was traditionally known (“Iran” is the Farsi word for “Land of the Aryans”). By the mid-nineteenth century, the region had been absorbed into Persia, but its sheikhs enjoyed semi-independence from Tehran. When the shah’s father, Reza Shah Pahlavi, took power (with British backing) in 1925, he set about “Persianizing” the region, a policy his son intensified: Farsi replaced Arabic as the official language, Iranian nationalists settled in the thousands, and senior official positions were filled by Farsi-speaking Persian Iranians. The province was renamed Khuzestan, an Iranian name. Arab opposition was suppressed. This Persianizing policy was motivated by power politics and ethnic prejudice but mostly by greed: for beneath the region’s desert sands bubbled a vast ocean of oil. Had fate dealt differently with the region, it might have become another Gulf oil state, like Qatar or Kuwait, with a small Arab population, and a lot of money. Instead, its oil riches bankrolled the shahs, exploited in concert with the British, then with the Americans. The expensive rugs and chandeliers in Iran’s London embassy were paid for with Khuzestan’s oil. At the height of the shah’s power, some five million barrels were being exported from the province daily, about one-tenth of the world’s entire oil trade.
The Arabs of Arabistan supported the replacement of the Shah by the Ayatollah Khomeini and the establishment of an Islamic Republic, but ended up disappointed.
Most of his fellow Arabs were illiterate, Towfiq complained, workhorses made to toil for their Iranian bosses: “We are very rich in resources, but it is taken away from Arabistan.” Only a handful of Arabs worked in the Iranian civil service; no Arab rose above the rank of captain in the armed forces. Fascinated by foreign culture, hungry for learning, Towfiq won a place to study English language and literature at the University of Tehran. “I am a rare case,” he said. “Out of four million people, we are only four thousand university graduates.” There he eagerly joined the students demonstrating against the shah.
But the ayatollah was no more willing than the shah to countenance self-government for oil-rich Khuzestan. Arabs were not the only ethnic minority agitating for greater self-determination. Kurds, Turkmens, Azeris, and Baluchis all sought to loosen Tehran’s grip, some by democratic means, others through violence. If the Arabs won autonomy, other groups would demand the same, threatening the very integrity of the country. “The new leaders forgot all their promises,” said Towfiq. The ayatollah clamped down on the Arabs, just as the shah had done.
Saddam Hussein, de facto ruler of Iraq since 1968 and president since 1979, spotted an opportunity in the unrest. A secular nationalist with pretensions to lead the Arab world, Saddam saw Iran’s aggressive new theocracy as a threat to his power and ambitions. Inciting rebellion among the Arabs of neighboring Khuzestan was an easy and cheap way to undermine the ayatollah and destabilize Iran, while also demonstrating Saddam’s credentials as an Arab champion. Bands of Iranian Arabs were trained in Iraq, armed, and sent back across the border to attack police stations, military checkpoints, roads, bridges, and above all the oil pipelines carrying Iran’s economic lifeblood. These Arab guerrillas saw themselves as fighters for independence, but they were dependent on Saddam Hussein, pawns cynically manipulated by the Iraqi leader for his own ends.
The conflict was racial as well as political, an ethnic confrontation between indigenous Arabs and Farsi-speaking Iranians introduced by the shahs to Persianize the region. Iranian militiamen flown in from Tehran roamed the streets in search of insurgents. Some fought back. Armed Arabs attacked a naval base, the central police station, government buildings, and shops. Three days of street fighting left 220 people dead and 600 wounded. The ayatollah’s secret police, the successors to SAVAK and no less vicious, set about hunting down Arab activists, many of whom were tried in hastily convened Revolutionary Courts and summarily executed. Ayatollah Sheikh Muhammad-Taher al-Khaqani, spiritual leader of the region’s Arabs and Khomeini’s former teacher, was arrested, along with hundreds of others. Those who escaped fled to Iraq or went into hiding.
The British have to figure out what to do, difficult since they didn’t have a significant stake in the fight and the European track record of dealing with Arab/Muslim terrorists wasn’t great:
In 1972, Palestinian terrorists of the Black September group seized Israeli athletes during the Munich Olympic Games. The West German handling of that incident had been a disaster, ending in the deaths of all the hostages and most of the terrorists.
Looking at the UK today, it’s tough to imagine that Margaret Thatcher ever existed, but of course she did.
As always, Thatcher made her opinions abundantly clear: she had “no intention of allowing terrorists to succeed in their hostage-taking,” as she wrote in her memoirs. “This was no less an attempt to exploit perceived Western weakness than was the hostage-taking of the American Embassy personnel in Tehran.” The Iron Lady was not for turning, in this or any other way, and her mind was already made up. “My policy would be to do everything possible to resolve the crisis peacefully, without unnecessarily risking the lives of the hostages, but above all that terrorism should be—and should be seen to be—defeated.” In any case, the gunmen were demanding something she could not deliver: the release of political prisoners in another, hostile country. The terrorists, whoever they were and whatever the eventual outcome, had committed a crime on British soil, and would be tried under English law.
Thatcher is just the sort of person to call in the SAS (Special Air Service) and a lot of the book covers the glorious history, training, and capabilities of the SAS (tough to imagine today given that the UK has been conquered without a shot having been fired).
The book goes into a lot of detail about the evolution of the relationship among five groups of people (1) hostage takers, (2) Iranian diplomats, (3) Iranian employees of the embassy who weren’t necessarily passionate about the Islamic regime, (4) visitors to the embassy, e.g., from Syria and Pakistan, (5) a few white British people. Most of them can find common ground in shared hatred of Israel/Jews and the hostage takers begin to soften when they realize that, with a couple of exceptions, the hostages aren’t tightly coupled to the new Islamic government in Iran.
Without giving too much of the story away, let me highlight that at least one of the hostage takers survived and was imprisoned.
Nejad was finally released in 2008, having served twenty-seven years. In Iran, he still faced murder charges for the deaths of Lavasani and Samadzadeh. Tehran gave no assurances he would not be tortured and executed if repatriated. He was therefore allowed to remain in the UK, a decision described by Iran as “condemnable and indefensible.” Fowzi Nejad now lives in the UK.
In other words, British law requires that the British welcome as a neighbor a foreigner who was convicted of one of the most spectacular crimes in modern British history. Prior to the siege of the embassy, he had never been to the UK. He traveled to the UK only to commit the crime of taking hostages. He never claimed to have any affinity for British culture, other than its perceived softness on terrorists, or the British people.
More: Read The Siege.
Arabistan/Kuzestan:
Full post, including comments